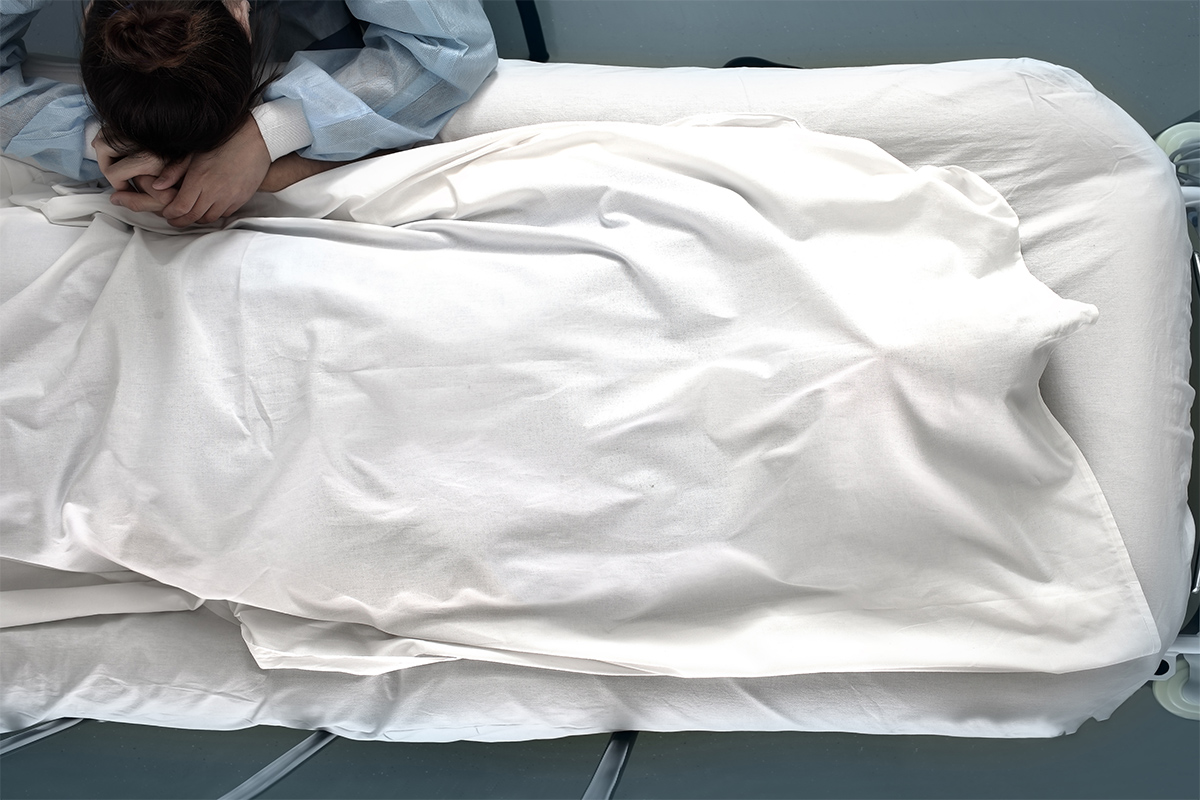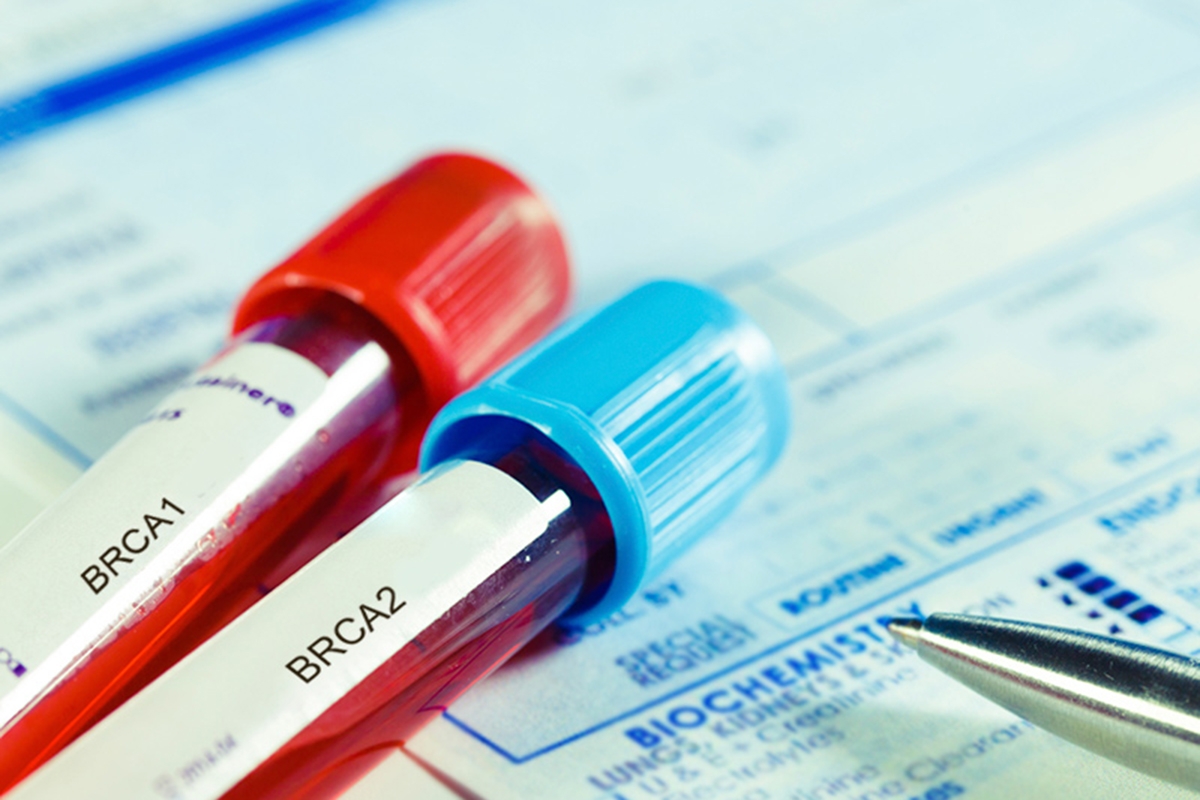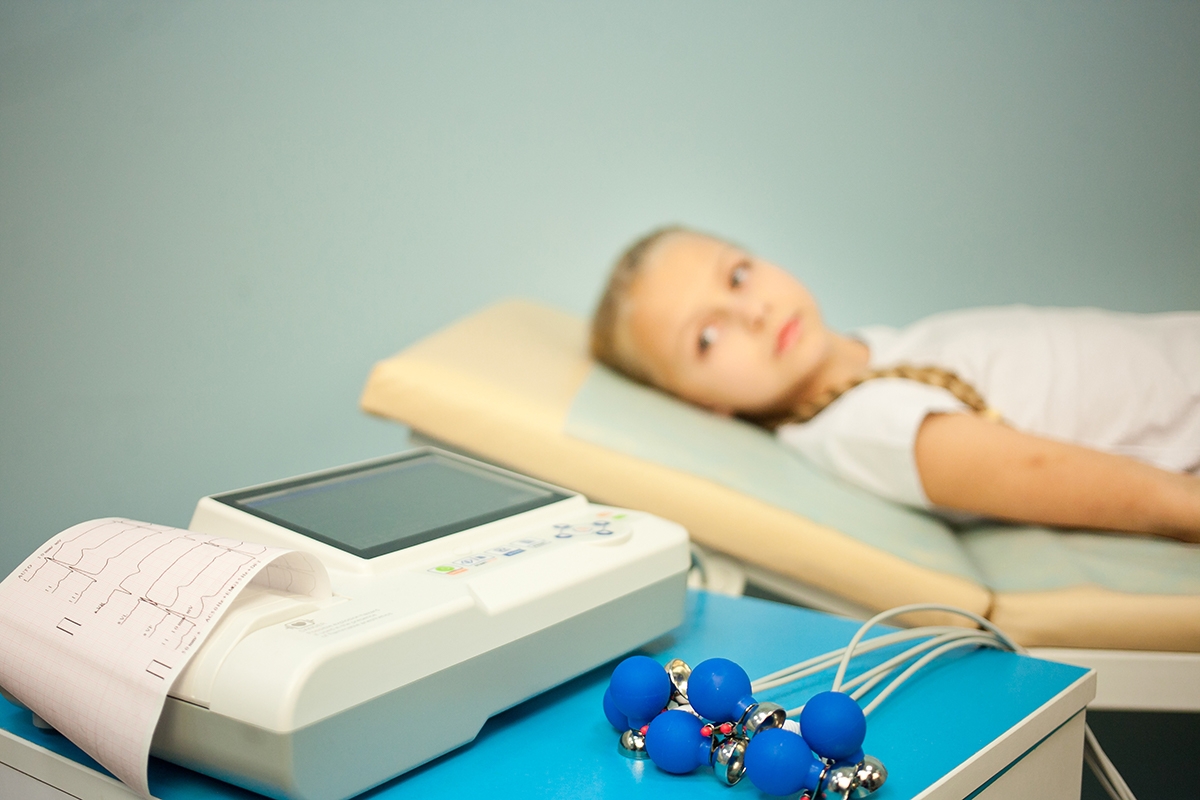
When technologically advanced medicine fails to “rescue [a patient] intact from the conditions of her birth,” professionals must rely even more squarely on the foundation of good medicine – human-centered caring. While we do not disagree with Mr. Teti’s ethical analysis, we believe that ethics consultants can (and should) do more to support the medical team in achieving this foundational goal.